Research in home NIV for COPD
Discover key findings from recent clinical research and their implications for treatment decision-making and patient selection.
What are the evidence based benefits of home NIV for COPD?
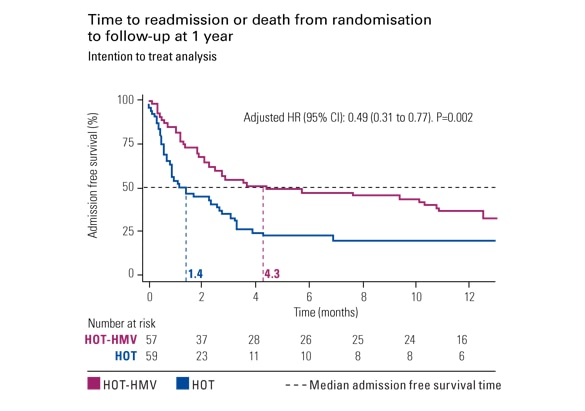
The HOT-HMV study
The HOT-HMV study1 has shown a 51% reduction in risk of hospital readmission or death in hypercapnic COPD patients treated with home non-invasive ventilation and oxygen therapy.
Patient monitoring
Careful monitoring is essential for patients initiated on high-intensity NIV.
This could be facilitated by telemedicine technology providing ventilatory data, patient-ventilator asynchrony, transcutaneous gas measures and other relevant parameters.

[Webinar] Home NIV in stable COPD: how and why?
With over 20 years of experience in the field of non-invasive ventilation, Professor Windisch explores the evolution of the treatment from early negative studies using low intensity pressure ventilation to today’s evidence based approach to improve survival and quality of life in patients with stable hypercapnic COPD.
Support for investigator initiated research
Resmed believes in the need to support ethical, independent clinical research, conducted by qualified third-party investigators.
References:
*As shown by 3 and 6 months results on quality of life and compliance
- Murphy P et al. Effect of Home Noninvasive Ventilation With Oxygen Therapy vs Oxygen Therapy Alone on Hospital Readmission or Death After an Acute COPD Exacerbation. A Randomized Clinical Trial, JAMA. Published online May 21, 2017. doi:10.1001/jama.2017.4451.
- Murphy PB et al. Cost-Effectiveness of Home Oxygen Therapy-Home Mechanical Ventilation (HOT-HMV) for the Treatment of Chronic Obstructive Pulmonary Disease (COPD) with Chronic Hypercapnic Respiratory Failure Following an Acute Exacerbation of COPD in the United Kingdom (UK). American Journal of Respiratory and Critical Care Medicine 2018;197:A2517.
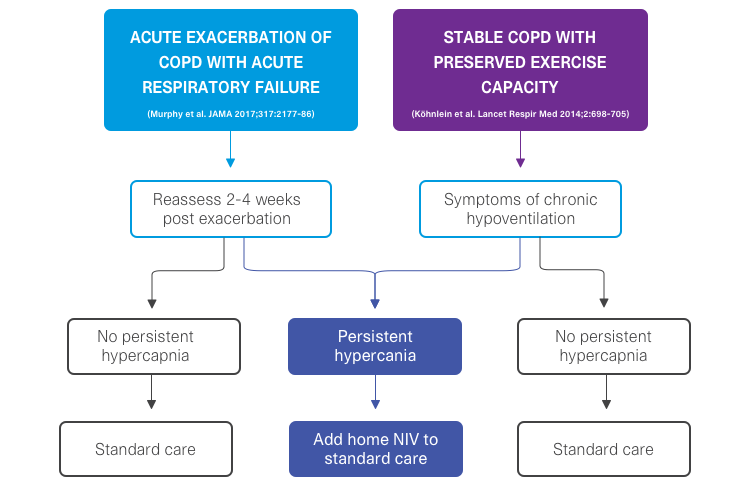
- Köhnlein T, et al., Non-invasive positive pressure ventilation for the treatment of severe stable chronic obstructive pulmonary disease: a prospective, multicentre, randomised, controlled clinical trial. Lancet Respir Med 2014;2:698-705.
- Struik FM, et al. Nocturnal non-invasive ventilation in COPD patients with prolonged hypercapnia after ventilatory support for acute respiratory failure: a randomised, controlled, parallel-group study. Thorax 2014;69:826-34.
- Vogelmeier DF, et al. Global strategy for diagnosis, management, and prevention of COPD. Am J Respir Crit Care Med 2017;195:557-82.
- Ergan B, Oczkowski S, Rochwerg B, et al. European Respiratory Society Guideline on Long-term Home Non-Invasive Ventilation for Management of Chronic Obstructive Pulmonary Disease. Eur Respir J 2019; in press (https://doi.org/10.1183/13993003.01003-2019).
- Nocturnal non-invasive positive pressure ventilation for COPD. Windisch W et al. Expert Rev Respir Med. 2015 Jun; 9(3):295-308.
- Dreher M, et al. Noninvasive ventilation in COPD: impact of inspiratory pressure levels on sleep quality. Chest 2011;140:939-45.