Treatment options for snoring
At ResMed, we have solutions for throat snorers with and without obstructive sleep apnoea. This includes mild to moderate OSA as well as more severe cases of OSA.
Throat snorers without sleep apnoea
Your patients fall into this category if they’ve tested for sleep apnoea and obtained an Apnoea-Hypopnoea Index (AHI) score of less than 5. If you don’t know what your patient’s AHI level is, we recommend you perform a sleep test, or refer them to a colleague who can. Understanding your patient’s sleep apnoea conditions will allow you to make optimal treatment choices.
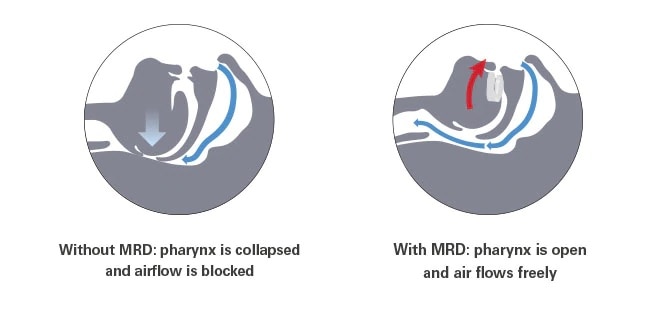
At ResMed, we believe that one of the most efficient treatment options for throat snoring is a custom-made Mandibular Repositioning Device (MRD) like Narval CC™.1,2 These oral appliances, which go by many names — mandibular advancement devices, intraoral devices, oral appliances, and mandibular repositioning devices — work by holding the lower jaw in a position during sleep that reduces the collapse of the airway and expands the space behind the tongue, to help prevent apnoea and snoring.
Narval CC not available in England, Wales and Scotland.
Is your patient a nose snorer? Then MRDs are not recommended; they won’t solve your patient’s problem. We invite you to investigate options that include sprays, nose strips, chin straps and more. Visit your country’s sleep association for recommendations.
Throat snorers with mild to moderate OSA
If your patient’s AHI levels fall between 5 and 30, ResMed offers both the Narval CC oral appliance as well as a full range of CPAP (Continuous Positive Airway Pressure) therapy options. MRDs are a clinically-proven alternative to CPAP therapy for snorers with mild to moderate OSA.3,4,5 They have higher levels of acceptance, so users are less likely to drop out of treatment.4 Among regular users, they are almost as effective as CPAP in reducing AHI levels.6
Throat snorers with severe OSA
If your patients’ AHI levels are over 30, you’ll no doubt recommend Positive Airway Pressure (PAP) therapy as a first choice. There are different types of PAP therapy, including:
- APAP (Automatic Positive Airway Pressure),
- CPAP (Continuous Positive Airway Pressure),
- Bi-level therapy.
ResMed has a full range of masks, devices and accessories to make PAP therapy as comfortable and non-intrusive as possible.
Some patients can struggle to adapt to CPAP therapy. If therapy adherence is a problem, you may wish to prescribe an MRD instead. In the largest multicentre study of its kind, users with severe OSA who regularly wore Narval CC were just as likely to reduce their AHI levels by 50% as wearers with mild to moderate OSA.1
Other options to stop snoring include surgery and radiofrequency treatment.
Clinical results for Narval CC: the ORCADES study
Evaluating the efficacy and compliance of the Narval CC MRD: that is the purpose of the ORCADES study, the largest multicentre trial of patients with obstructive sleep apnoea-hypopnoea syndrome (OSAHS) who are being treated with a custom-made MRD. The ongoing study follows 369 patients over a period of 5 years.1 158 patients – 43% of the study participants – have severe OSAHS (AHI>30).

More about treatment options

Treatment options for OSA
ResMed offers a range of effective treatment options for OSA, including CPAP, APAP, bilevel therapy and oral appliance therapy.

Treatment options for CSA
Adaptive servo-ventilation (ASV)* is an appropriate choice for treating most of these more complex patients.

Digital health for sleep apnoea
ResMed connected solutions enable pro-active monitoring by healthcare professionals and result in more responsible patients who are involved and interested in their sleep apnoea therapy.
References:
* ASV therapy is contraindicated in patients with chronic, symptomatic heart failure (NYHA 2-4) with reduced left ventricular ejection fraction (LVEF ≤ 45%) and moderate to severe predominant central sleep apnoea.
- Vecchierini MF & al. A custom-made mandibular repositioning device for obstructive sleep apnoea-hypopnoea syndrome: the ORCADES study. Sleep Med. 2016 Mar;19:131-40. doi: 10.1016.
- Lim et al. Oral appliances for OSA. Cochrane Database of Systematic Reviews 2009, Issue 3.
- Practice Parameters for the Treatment of Snoring and Obstructive Sleep Apnea with Oral Appliances: An Update for 2005, AASM report, Sleep 2006;29(2): 240-243, US Guidelines.
- Non-CPAP therapies in obstructive sleep apnoea, ERS task force. Eur Respir J. 2011 May;37(5):1000-28, Systematic Review. Recommendations (European).
- B. Fleury et al. OSAHS treatment with mandibular advancement oral appliance. Rev Mal Respir. 2010 Oct;27 Suppl 3:S146-56. Systematic Review. Recommendations (France).
- Vanderveken OM. Objective measurement of compliance during oral appliance therapy for sleep-disordered breathing. Thorax. 2013 Jan;68(1):91-6.
